
Eosinophilic Granulomatosis with Polyangiitis
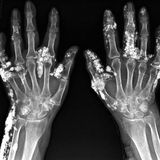
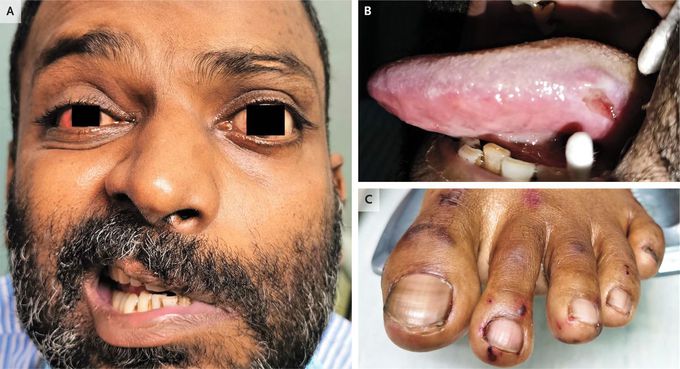
A 42-year-old man presented to the ophthalmology clinic with 5 days of pain and redness in both eyes. He reported no history of asthma but had recently received a diagnosis of otitis media and sensorineural hearing loss at the otolaryngology clinic. Physical examination showed anterior scleritis in the right eye, episcleritis in the left eye, facial-nerve palsy on the left side (Panel A), a large ulcer on the lateral side of the tongue (Panel B), and hemorrhagic petechiae on both feet, including the toes (Panel C). Laboratory studies showed an absolute eosinophil count of 2220 per cubic millimeter (reference range, 20 to 500), positivity for perinuclear antineutrophil cytoplasmic antibody, and a proteinase 3 antibody concentration of 237 U per milliliter (reference value, <18). Biopsy of skin from the foot revealed leukocytoclastic vasculitis with marked perivascular infiltration of eosinophils mixed with neutrophils. A diagnosis of eosinophilic granulomatosis with polyangiitis was made. All the antineutrophil cytoplasmic antibody–associated vasculitides may involve the eyes, peripheral nerves, skin, and oral mucosa, but eosinophilic granulomatosis with polyangiitis is typically distinguished by the presence of asthma and tissue and peripheral eosinophilia. Treatment with systemic glucocorticoids and cyclophosphamide was initiated, and at 6 months of follow-up, all the patient’s symptoms except the facial droop had resolved. Geng-Yi Yong, F.R.C.Ophth. University of Malaya, Kuala Lumpur, Malaysia

