

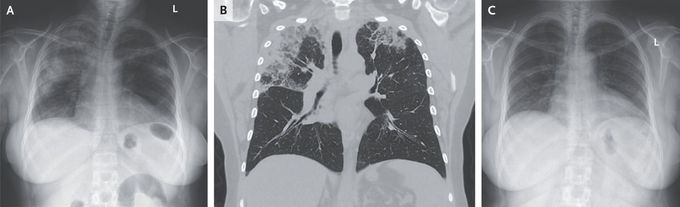
“Photographic Negative of Pulmonary Edema” in Chronic Eosinophilic Pneumonia
A 54-year-old woman with asthma and allergic rhinitis presented to the emergency department with a 3-month history of productive cough and dyspnea. She also reported fevers, chills, night sweats, and an unintentional 9-kg (20-lb) weight loss. Her medications were montelukast, cetirizine, and an albuterol inhaler. She was a lifelong nonsmoker and had not traveled recently. On lung examination, there was expiratory wheezing and diffuse crackles. Laboratory testing showed an absolute eosinophil count of 5240 per cubic millimeter (reference range, 40 to 360). A chest radiograph showed peripheral airspace opacities on both sides (Panel A). Subsequent computed tomography of the chest showed upper lobe–predominant peripheral and subpleural consolidations that spared the perihilar region (Panel B). The radiographic pattern was described as a “photographic negative of pulmonary edema” — a finding suggestive of chronic eosinophilic pneumonia. Serum testing for IgE against Aspergillus fumigatus, antibodies against coccidioides, and antineutrophil cytoplasmic antibodies was negative. Bronchoscopy with bronchoalveolar lavage was notable for 74% eosinophils in the cell count (reference value, <2) and negative tests for infectious diseases. A diagnosis of chronic eosinophilic pneumonia was made. Treatment with oral prednisone was started. At follow-up 17 days later, the patient’s symptoms had abated and the radiographic findings had resolved (Panel C). The patient continued to take prednisone for 5 months and had no further flare-ups.

