

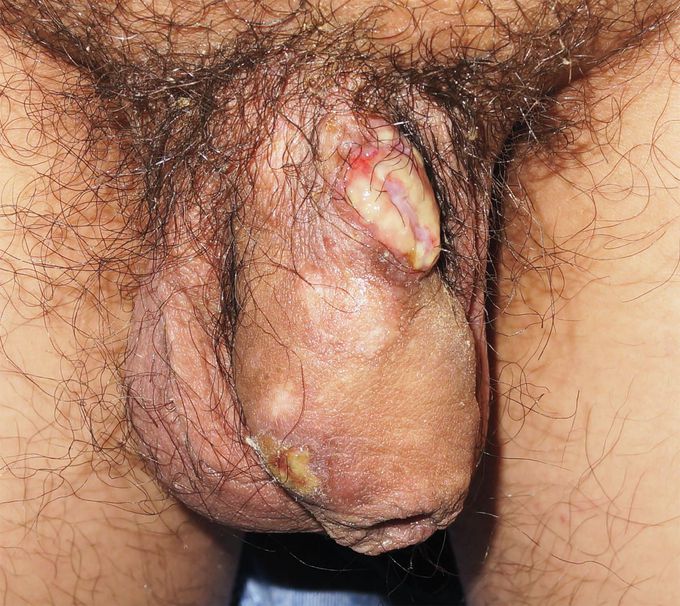
Herpes Vegetans
A 39-year-old man with human immunodeficiency virus (HIV) infection that was being treated with antiretroviral therapy presented to the dermatology clinic with a 1-year history of recurrent, painful penile ulcers. Approximately once per month, erosions would appear on his penile shaft, ulcerate, heal without specific treatment, and then recur. On physical examination, there were two exophytic plaques with central ulceration and raised borders. There were also hypopigmented patches at the sites of healed lesions. Laboratory testing showed a CD4 cell count of 494 per cubic millimeter (reference range, 414 to 1123) and an HIV viral load of 450 copies per milliliter (reference range, <20). Biopsies of the lesions revealed epidermal necrosis, pseudoepitheliomatous epidermal hyperplasia, and a dense infiltrate of inflammatory cells in the dermis and subcutaneous tissue. A next-generation sequencing assay to detect sexually transmitted infection (STI) identified herpes simplex virus (HSV) type 2. Other microbiologic testing was negative. A diagnosis of herpes vegetans was made. Herpes vegetans — also known as hypertrophic herpes simplex — is an uncommon manifestation of HSV infection seen in persons with immunocompromise. It manifests as verrucous, proliferative, or ulcerative lesions, often with a chronic, persistent course. Treatment with oral valacyclovir was given. Screening for other STIs was negative. At a 2-week follow-up, the lesions had abated.
Living with HIV was one of the hardest experiences of my life. The fatigue, the emotional toll, and the uncertainty about the future weighed on me every single day. I had tried many treatments and medications, but nothing seemed to restore my health or energy the way I hoped.Out of both hope and desperation, I came across NaturePath Herbal Clinic. At first, I was skeptical but something about their natural approach and the powerful stories I read gave me the courage to try one more time.I began their herbal treatment program, and within a few weeks, I noticed small but meaningful changes more energy, better sleep, and a stronger immune system. Over the months, those improvements only grew. Today, I can truly say my life has changed. I feel healthier, more balanced, and finally in control of my well-being again.This isn’t just a testimony it’s a heartfelt recommendation to anyone living with HIV or any chronic condition. Don’t give up hope. I’m so grateful I gave NaturePath Herbal Clinic a chance. Visit their website to learn more: www.naturepathherbalclinic.com Email: info@naturepathherbalclinic.com
I'm super excited! I finally got rid of my HSV-1. I got diagnosed of herpes from my husband who never told me he had the virus. I got tested at first when i first had the virus and i My doctors prescribed Antiviral medicine for me which really helped me a lot in suppressing the virus. I finally got cured using herbal protocol ordered from Dr Oyagu an African herbalist. I used his Products and it completely fought the virus and was tested negative. You can DM the herbalist for help if needed. via email oyaguherbalhome@gmail.com His medicine is 100% strong and active in eliminated herpes permanently. I can 't explain my feelings right now. I'm supper excited.



