

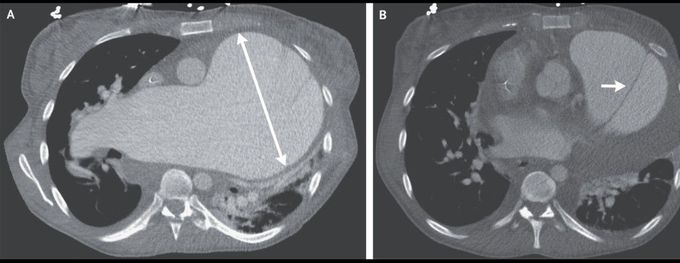
Pulmonary-Artery Aneurysm with Acute Dissection
A 35-year-old woman with idiopathic pulmonary arterial hypertension presented to the emergency department with a 1-day history of chest pain. She had been undergoing evaluation for lung transplantation and was known to have a 12-cm pulmonary-artery aneurysm that had been enlarging over the preceding 8 years (Panel A). The heart rate was 101 beats per minute, the blood pressure 109/66 mm Hg, and the oxygen saturation 97% while the patient was receiving 4.5 liters of oxygen per minute. A computed tomographic scan of the chest showed a new dissection flap originating in the main pulmonary artery and extending into the left pulmonary artery (Panel B, arrow). She was admitted to the hospital, where the medications she had been taking — tadalafil, macitentan, and infused treprostinil — were continued, and was listed for urgent lung transplantation. On the day after admission, the hypoxemia worsened and new onset of atrial fibrillation with a rapid ventricular response was observed. Venoarterial extracorporeal membrane oxygenation was initiated and was continued for 2 days, at which time the patient underwent transplantation of both lungs and replacement of the main pulmonary artery and pulmonary valve. Pulmonary-artery dissection is a rare complication of long-standing pulmonary hypertension. Patients may present with worsening chest pain, dyspnea, or shock. The patient was discharged 2 weeks after transplantation and continued to do well 6 months later at follow-up.

