

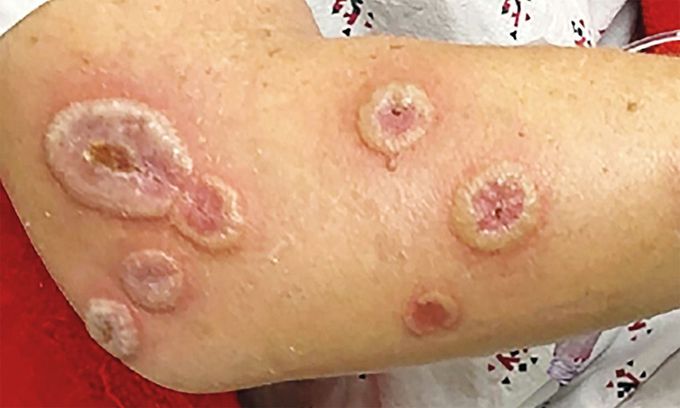
Acute Febrile Neutrophilic Dermatosis
A 46-year-old woman presented to the emergency department with an erythematous lesion on her left thumb that had developed over the course of 2 days. She received a diagnosis of acute paronychia and was treated with oral clindamycin. By day 7 of treatment, the initial lesion had increased in size, and multiple painful, circular, raised lesions with central erosion and crusting had developed on her face, feet, hands, and arms. She reported no recent viral or other infections and had neither current nor previous gastrointestinal symptoms suggestive of inflammatory bowel disease. Laboratory studies showed a leukocyte count of 11,700 per cubic millimeter (reference range, 4100 to 10,700) and a normal glycated hemoglobin level. Tests for antinuclear antibodies, antineutrophil cytoplasmic antibodies, human immunodeficiency virus antibodies, and syphilis were all negative, as was evaluation for viral hepatitis. A biopsy specimen of one of the lesions showed a neutrophilic inflammatory infiltrate that was consistent with acute febrile neutrophilic dermatosis, also known as Sweet’s syndrome. This inflammatory condition can mimic an infectious process and is important to consider, especially in cases in which cutaneous lesions do not abate with antibiotic treatment. Oral prednisone was initiated, and the pain, as well as the discoloration and size of the lesions, decreased within 48 hours. At a 1-month follow-up visit, the inflammation had resolved, with some mild residual skin discoloration.

