

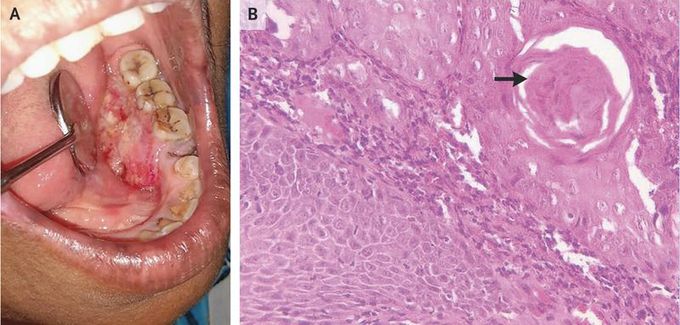
Squamous-Cell Carcinoma of the Mouth
A 54-year-old woman presented to a dental clinic with a 1-year history of oral swelling and a sore mouth. She had regularly chewed loose-leaf tobacco, which she had placed on the floor of her mouth between the jaw and tongue, up to five times each day for more than 10 years. Intraoral examination revealed an irregular, indurated lesion that measured 3 cm in its greatest dimension and was located on the floor of the mouth inside the left jaw (Panel A). Incisional biopsy of the lesion revealed invasive squamous-cell carcinoma with hyperchromic, pleomorphic cells and a “keratin pearl” (Panel B, arrow) in the connective tissue. Computed tomography and positron-emission tomography showed no bony or lymph-node involvement. Squamous-cell carcinoma is the most common type of neoplasm of the oral cavity. The patient underwent an en bloc excision of the carcinoma as well as segmental mandibulectomy with the use of a vascularized free fibular flap as an osteocutaneous graft and selective neck dissection. Pathological analysis revealed no involvement of bone or lymph nodes, with tumor-free margins. The patient was advised to stop using tobacco products. Two years after treatment, she remained free of recurrence.


