

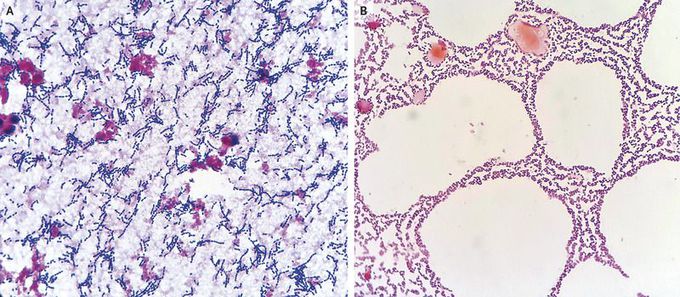
Pneumococcal Bacteremia and Meningitis
A 64-year-old man with human immunodeficiency virus infection, type 2 diabetes, and a history of splenectomy after trauma presented to the emergency department with confusion, headache, and fever. He had not been receiving regular medical care and took no medications. His vaccination history after splenectomy was unknown. On physical examination, the patient had hypotension, tachycardia, neck stiffness, and Brudzinski’s sign. Laboratory tests showed a white-cell count of 14,900 per cubic millimeter (normal range, 4000 to 11,000) and a platelet count of 38,000 per cubic millimeter (normal range, 140,000 to 400,000). Gram’s stain of an aliquot of blood removed from a culture bottle of the patient’s blood after 1.5 hours of incubation (Panel A) and of the patient’s cerebrospinal fluid (directly without culture) (Panel B) revealed abundant gram-positive cocci in pairs and chains. A diagnosis of fulminant pneumococcal sepsis was made. Sepsis can be rapidly fatal in patients with asplenia. Streptococcus pneumoniaeis an encapsulated organism that is removed by immunoglobulin-mediated opsonization by phagocytes that reside primarily in the spleen. Asplenia leads to diminished antibody-mediated phagocytosis, increasing the vulnerability of the host to encapsulated pathogens. The patient was admitted to the intensive care unit and was treated with intravenous vancomycin, ceftriaxone, and immune globulin. Despite initial stabilization of the patient’s blood pressure, severe cognitive impairment developed, and he was transferred to hospice care.

