

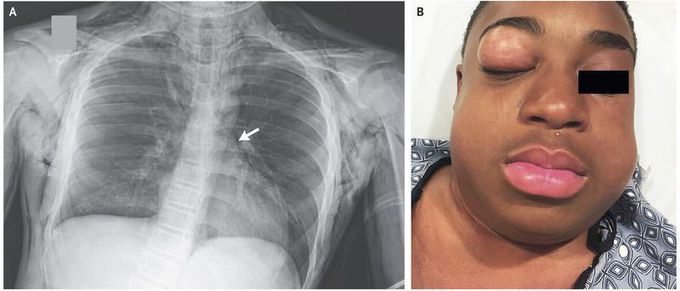
Diffuse Subcutaneous Emphysema
A 14-year-old boy with a history of asthma presented to the emergency department with a 1-day history of wheezing and coughing. His initial oxygen saturation was 83% while he was breathing ambient air, and the physical examination was notable for diffuse wheezing and the use of accessory muscles of ventilation. He received albuterol, ipratropium, intravenous magnesium, and intravenous glucocorticoids and was admitted to the hospital for a severe asthma exacerbation. Two days later, he had worsening respiratory distress and wheezing and was transferred to the pediatric intensive care unit for continuous albuterol treatment. Swelling and crepitus of the neck also developed. Among the findings on his chest radiograph was a pneumomediastinum (Panel A, arrow) with diffuse subcutaneous emphysema. Four days later, as his respiratory status improved, sudden swelling and palpable crepitus developed in both cheeks and the right eyelid (Panel B). He had no associated eye pain or diplopia, and extraocular movements were intact. Palpebral emphysema can occur as a complication of pneumomediastinum and typically resolves without intervention. On hospital day 7, the patient’s asthma exacerbation resolved and he was discharged home with intermittent albuterol treatment and a tapering course of prednisone. The eyelid swelling resolved slowly over 2 weeks.

