

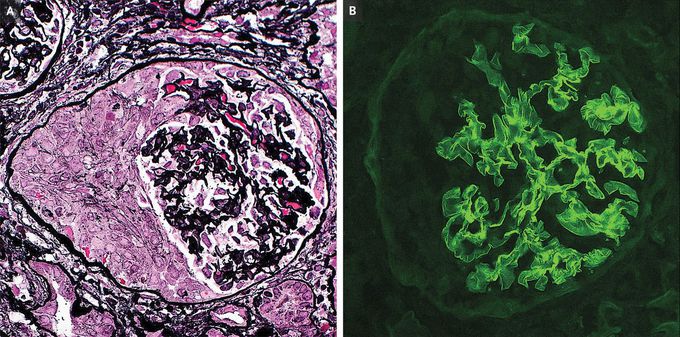
Anti–Glomerular Basement Membrane Glomerulonephritis
A 60-year-old woman with hypertension and chronic kidney disease of unknown cause was referred to the emergency department because of a serum creatinine level of 7.8 mg per deciliter (reference range, 0.5 to 0.9). At baseline, her creatinine level had been 1.6 mg per deciliter. Before presentation, she had been feeling well. The vital signs and physical examination were normal. A urinalysis showed 2+ protein and more than 180 red cells per high-power field, and no urinary casts were seen. A chest radiograph was normal. Her kidney function did not improve with administration of intravenous fluids, and therefore further evaluation was performed. Tests for antineutrophil cytoplasmic antibody, antinuclear antibody, and complement levels were normal, but an indirect fluorescent antibody assay for anti–glomerular basement membrane (GBM) antibodies was positive. A subsequent kidney biopsy showed crescentic glomerulonephritis (Panel A) with strong linear GBM staining for IgG on immunofluorescence (Panel B). A diagnosis of anti-GBM glomerulonephritis was made. Although anti-GBM disease can involve both the kidneys and the lungs, older patients more often present with isolated kidney involvement. Treatment with plasma exchange, glucocorticoids, and cyclophosphamide was initiated. Anti-GBM antibodies were undetectable by day 3 of plasma exchange, but the patient remained dialysis-dependent at the 6-month follow-up.

