

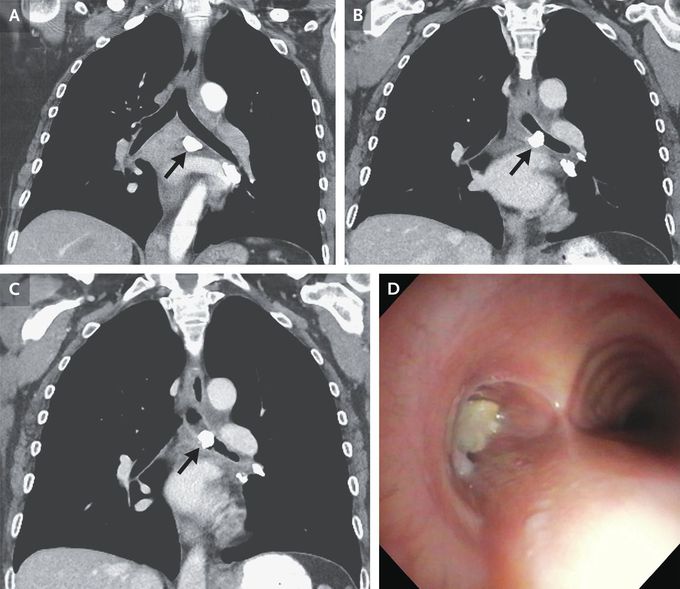
Broncholithiasis
A 53-year-old woman with a history of metastatic lung adenocarcinoma presented to the pulmonary clinic with a 3-month history of progressive shortness of breath and cough. Her lung cancer had been in partial remission. Computed tomography (CT) of the chest was performed. When previous CT images of the chest were compared with those from the current presentation (Panel A, 15 months before presentation; Panel B, 3 months before presentation; Panel C, current presentation), a calcified subcarinal lymph node (Panels A, B, and C, arrow) was noted to have migrated into the left mainstem bronchus. A diagnosis of broncholithiasis was made. Broncholithiasis occurs when calcified material — typically a mediastinal lymph node — erodes into a bronchus, causing cough, dyspnea, hemoptysis, or even expectoration of broncholith fragments (also known as lithoptysis). The most common cause of these calcified lymph nodes is previous granulomatous infection, presumed to be histoplasmosis in this patient, since histoplasmosis is common in Iowa, where this patient lived. The patient was referred to the interventional pulmonology section. During bronchoscopy, the broncholith was visualized in the left mainstem bronchus (Panel D). A holmium laser and rigid forceps were used to fracture the bronchlith into multiple pieces and remove it. Immediately after the procedure, the patient’s dyspnea and cough resolved. At the 6-month follow-up, she reported no recurrence of symptoms.

