

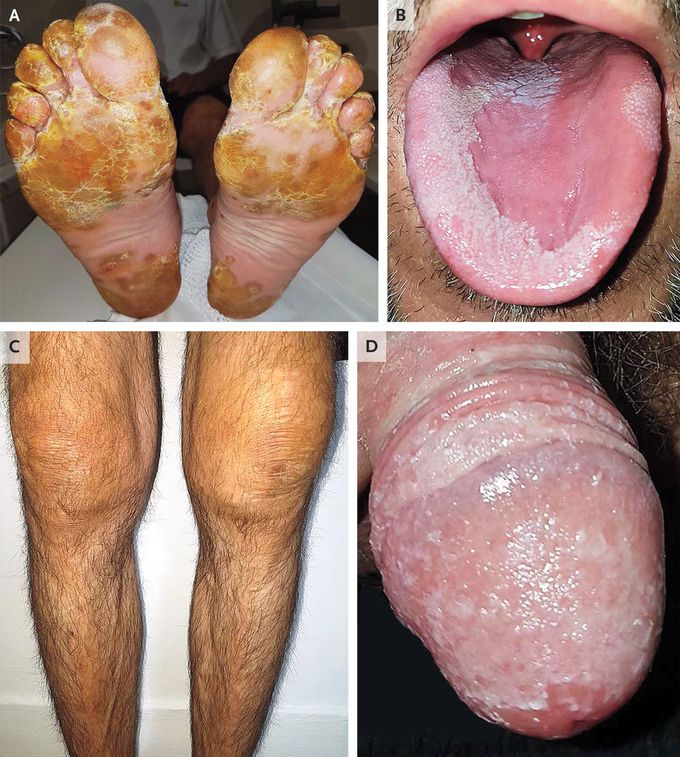
Reactive Arthritis
A 40-year-old man presented to the dermatology clinic with a 2-week history of a scaly foot rash, joint swelling, and low back pain. He had no known medical history but had had diarrhea and urethral discharge 7 days before the onset of his current symptoms. On examination, yellow pustules with hyperkeratosis consistent with keratoderma blenorrhagicum were noted on the plantar surfaces of his feet (Panel A). There were also new psoriatic skin lesions on his scalp, trunk, and dorsal hands, as well as pitting, hyperkeratosis, discoloration, and distal onycholysis on some nails. Other findings included conjunctivitis, migratory glossitis (Panel B), swelling of both knees (Panel C) and the right ankle, and circinate balanitis (Panel D). The C-reactive protein level was 59 mg per liter (reference value, <5), and a urine test was positive for sterile pyuria. Results of an analysis of left-knee synovial fluid were consistent with noninfectious inflammatory arthritis. Tests for rheumatoid factor, Chlamydia trachomatis, and other infectious agents were negative. A diagnosis of reactive arthritis was made. The patient was referred to the rheumatology clinic, and subsequent testing for HLA-B27 was positive. After 5 months of treatment with nonsteroidal antiinflammatory agents, systemic glucocorticoids, and sulfasalazine, the patient’s symptoms abated.

