

Gingival Infiltration in Acute Monocytic Leukemia List of authorsIMAGES IN CLINICAL MEDICINE Gingival Infiltration in Acute Monocytic Leukemia
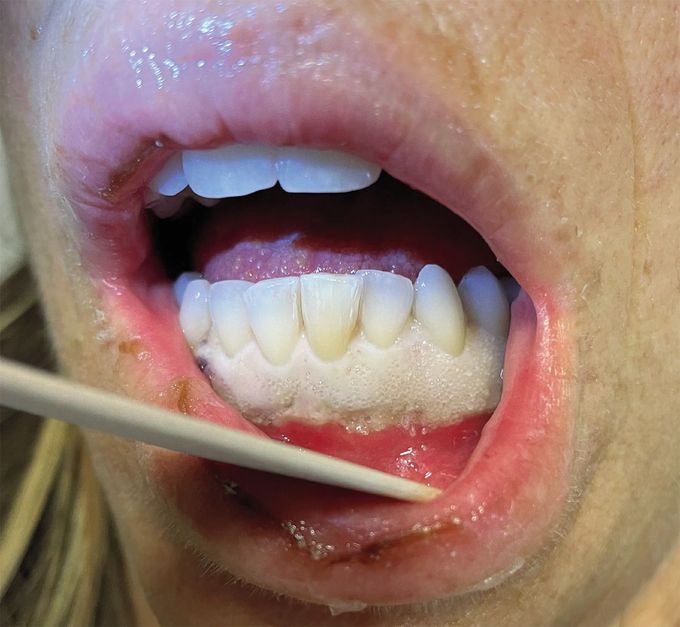
A 48-year-old woman presented to the emergency department with a 1-week history of fatigue and painful, swollen gums. Her temperature was 39.3°C, and her pulse was 114 beats per minute. On physical examination, there was a well-demarcated region of gingival infiltration and whitening, with submandibular lymphadenopathy on the right side. The white-cell count was 225,000 per cubic millimeter (reference range, 4800 to 10,800). A peripheral-blood smear showed myeloblasts with Auer rods, and flow cytometry revealed 89% blasts. A bone marrow biopsy also showed 89% blasts, with positive staining for CD34, CD117, and myeloperoxidase, confirming a diagnosis of acute monocytic leukemia. A chimeric trisomy 4 mutation was identified on cytogenetic analysis. No abnormalities were detected on next-generation sequencing. Gingival infiltration by leukemic cells may be a sign of acute myeloid leukemia, especially in patients with a monocytic subtype. After the initiation of treatment with hydroxyurea and chemotherapy, the gingival swelling abated and the leukemia went into remission. Since then, the patient has been receiving treatment with consolidation chemotherapy and undergoing evaluation for hematopoietic stem-cell transplantation.

