

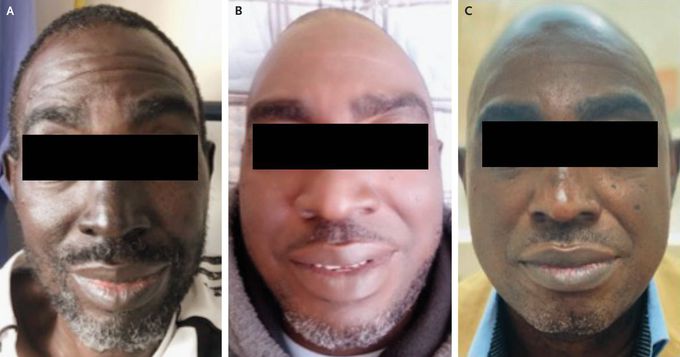
Hyperpigmentation from Addison’s Disease
A 54-year-old man presented to the emergency department with confusion and vomiting. Three months earlier, he had received a diagnosis of stage 4 chronic kidney disease. On examination, his blood pressure was 91/70 mm Hg and his pulse was 107 beats per minute. His abdomen was diffusely tender. Laboratory studies showed a serum glucose level of 40 mg per deciliter (2.2 mmol per liter; reference range, 70 to 110 mg per deciliter [3.9 to 5.6 mmol per liter]), a sodium level of 108 mmol per liter (reference range, 136 to 145), and a potassium level of 6.4 mmol per liter (reference range, 3.5 to 5.1). He also reported an unintentional weight loss of 10 kg and progressive darkening of the skin (Panel A) as compared with its appearance 6 months before presentation (Panel B). Hyperpigmentation was also noted in the gingival mucosa. The confusion and vomiting abated after fluid resuscitation and the resolution of hyponatremia and hypoglycemia. Further laboratory studies showed that insulin and C-peptide levels were appropriately suppressed at 0.3 mIU per liter (reference range, 2.6 to 24.9) and 0.4 μg per liter (reference range, 1.1 to 4.4), respectively. However, the early-morning cortisol level was 30 nmol per liter (reference range, 133 to 537) and the serum corticotropin level was 40.7 pmol per liter (reference range, 1.6 to 13.9). A diagnosis of primary adrenal insufficiency, or Addison’s disease, was made, and treatment with glucocorticoids and fludrocortisone was initiated. At follow-up 6 months after presentation, the patient noted a reduction in the hyperpigmentation (Panel C), and his weight had returned to its previous baseline.

