

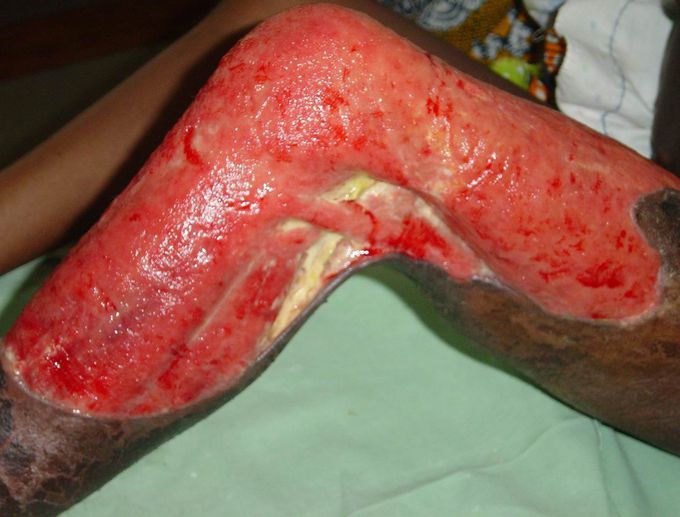
BURULI ULCER
Buruli ulcer, caused by Mycobacterium ulcerans, is a chronic debilitating disease that affects mainly affects the skin and sometimes bone. The organism belongs to the family of bacteria that causes tuberculosis and leprosy, which provides an opportunity for collaboration with these disease programmes. However, M. ulcerans is an environmental bacterium and produces unique toxin – mycolactone. The mode of transmission to humans remains unknown. Currently, early diagnosis and treatment are crucial to minimizing morbidity, costs and prevent long-term disability. Transmission Mycobacterium ulcerans grows at temperatures between 29–33 °C (Mycobacterium tuberculosis grows at 37 °C) and needs a low (2.5%) oxygen concentration. The organism produces a unique toxin – mycolactone – which causes tissue damage and inhibits the immune response. The exact mode of transmission of M. ulcerans is still unknown. Signs and symptoms Buruli ulcer often starts as a painless swelling (nodule), a large painless area of induration (plaque) or a diffuse painless swelling of the legs, arms or face (oedema). The disease may progress with no pain and fever. Without treatment or sometimes during antibiotics treatment, the nodule, plaque or oedema will ulcerate within 4 weeks. Bone is occasionally affected, causing deformities. The disease has been classified into three categories of severity: Category I single small lesion (32%), Category II non-ulcerative and ulcerative plaque and oedematous forms (35%) and Category III disseminated and mixed forms such as osteitis, osteomyelitis and joint involvement (33%). Lesions frequently occur in the limbs: 35% on the upper limbs, 55% on the lower limbs, and 10% on the other parts of the body. Health workers should be careful in the diagnosis of Buruli ulcer in patients with lower leg lesions to avoid confusion with other causes of ulceration such as diabetes, arterial and venous insufficiency lesion. Diagnosis In most cases, experienced health professionals in endemic areas can make a reliable clinical diagnosis but training is essential. Other conditions should be excluded from the diagnosis, including tropical phagedenic ulcers, chronic lower leg ulcers due to arterial and venous insufficiency (often in elderly populations), diabetic ulcers, cutaneous leishmaniasis, extensive ulcerative yaws and ulcers caused by Haemophilus ducreyi. Early nodular lesions are occasionally confused with boils, lipomas, ganglions, lymph node tuberculosis, onchocerciasis nodules or deep fungal subcutaneous infections. In Australia, papular lesions may initially be confused with an insect bite. Cellulitis may look like oedema caused by M. ulcerans infection but in the case of cellulitis, the lesions are painful and the patient is ill and febrile. HIV infection complicates the management of the patient, making clinical progression more aggressive and resulting in poor treatment outcomes. Four standard laboratory methods can be used to confirm Buruli ulcer: IS2404 polymerase chain reaction (PCR), direct microscopy, histopathology and culture. Treatment Treatment consists of a combination of antibiotics and complementary treatments. Treatment guidance for health workers can be found in the WHO publication Treatment of mycobacterium ulcerans disease (Buruli ulcer). A recent study suggests the combination of rifampicin (10 mg/kg once daily) and clarithromycin (7.5 mg/kg twice daily) is now the recommended treatment. In Australia, a combination of rifampicin (10 mg/kg once daily) and moxifloxacin (400 mg once daily) is routinely used with good results but its effectiveness has not been proven. Interventions such as wound and lymphoedema management and surgery (mainly debridement and skin grafting) are used to speed up healing, thereby shortening the duration of hospitalization. Physiotherapy is needed in severe cases to prevent disability. Those left with disability require long-term rehabilitation. These same interventions are applicable to other neglected tropical diseases, such as leprosy and lymphatic filariasis.
Fun fact: It’s called "Buruli" because Buruli is a place in Uganda where this ulcer happened a lot before they knew what it was
This was such a good review and even more so new info for me! Very thorough 😊
Living with HIV was one of the hardest experiences of my life. The fatigue, the emotional toll, and the uncertainty about the future weighed on me every single day. I had tried many treatments and medications, but nothing seemed to restore my health or energy the way I hoped.Out of both hope and desperation, I came across NaturePath Herbal Clinic. At first, I was skeptical but something about their natural approach and the powerful stories I read gave me the courage to try one more time.I began their herbal treatment program, and within a few weeks, I noticed small but meaningful changes more energy, better sleep, and a stronger immune system. Over the months, those improvements only grew. Today, I can truly say my life has changed. I feel healthier, more balanced, and finally in control of my well-being again.This isn’t just a testimony it’s a heartfelt recommendation to anyone living with HIV or any chronic condition. Don’t give up hope. I’m so grateful I gave NaturePath Herbal Clinic a chance. Visit their website to learn more: www.naturepathherbalclinic.com Email: info@naturepathherbalclinic.com




