

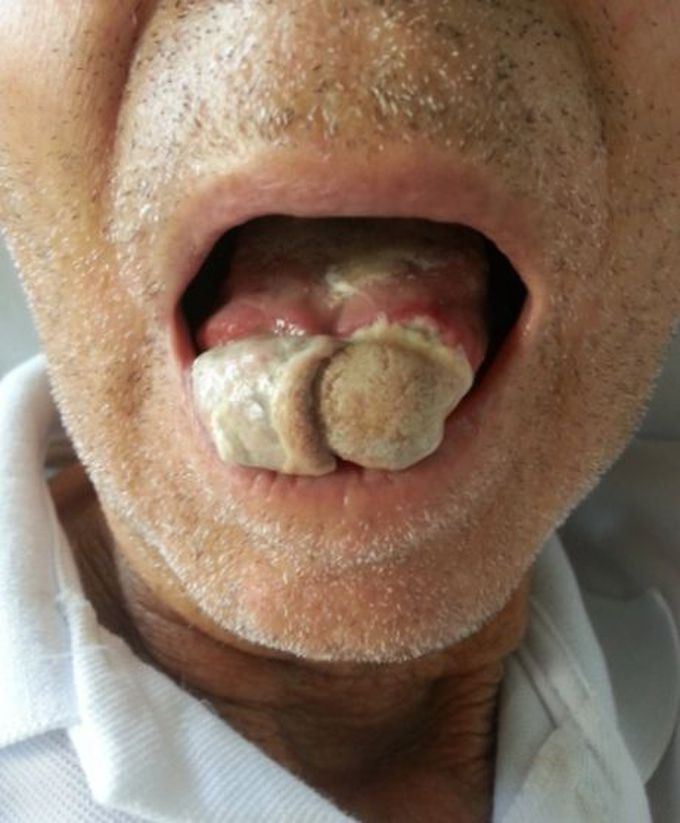
Lingual Necrosis - A rare manifestation of Giant Cell Arteritis
Giant Cell Arteritis (GCA) is a type of vasculitis which commonly involves medium and large sized vessels. Headache, jaw claudication, amaurosis fugax and vision loss are the most common symptoms seen in this condition but tongue necrosis is relatively rare, due to its rich vascular supply. Below is a case of 85 year old, hypertensive male, who presented in Emergency Department with a severe fronto-temporal headache along with jaw pain. The patient had been suffering from mild to moderate headache and jaw pain for the past 30 days. However, the headache increased in severity for the last 7 days along with jaw pain which involved floor of the mouth as well as the chin. Past medical history revealed cataracts and osteoporosis. The patient was suspected for GCA, on the second day of admission the patient suffered severe pain in the tongue and was not able to eat anything. On inspection, lingual volume was increased along with edema and white plaques. A lingual swab was taken which later revealed oral candidiasis. The patient was put on fluconazole therapy. Within 24 hours the color of tongue changed from white to grey, indicating lingual ischemia. Temporal pulses were absent and bilateral amaurosis was seen. Complete Blood count showed highly raised ESR and CRP as well as mild leukocytosis and anemia, indicating an acute inflammatory crisis. A doppler ultrasound and biopsy was taken which confirmed the diagnosis of Giant Cell Arteritis. The patient was put on 1mg/kg/day Prednisone followed by methotrexate 10mg/ week. After 14 days the necrotic area of the tongue detached itself on its own from the healthy tissue. Late, the Prednisone dose was tapered off to 20mg/kg gradually and the patient was discharged.
What was supposed to be done, had it been diagnosed earlier
Well, I would say that we could've stopped it by introducing the steroids earlier as disease severity would've been less than the current situation and patient would've had his tongue intact


