

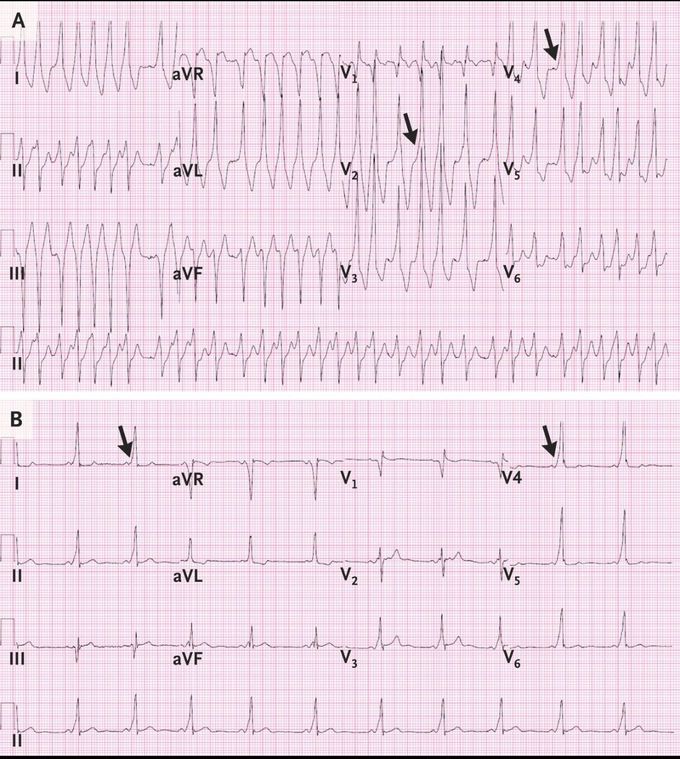
Preexcited Atrial Fibrillation after a Blood Draw
A 33-year-old man presented to the emergency department with palpitations after syncope occurred while a blood sample was being obtained. He had tachycardia, with a heart rate of 192 beats per minute in an irregularly irregular rhythm. An electrocardiogram (Panel A) showed wide-complex tachycardia with irregular RR intervals, delta waves (arrows), and no P waves, findings suggestive of preexcited atrial fibrillation. After the administration of 1 g of intravenous procainamide, a repeat electrocardiogram (Panel B) showed sinus rhythm with a short PR interval, a wide QRS complex, and delta waves (arrows), findings consistent with the Wolff–Parkinson–White syndrome. The Wolff–Parkinson–White pattern is seen in patients who have an accessory conduction pathway between the atria and the ventricles, in addition to the atrioventricular node. Preexcitation of the ventricular myocardium occurs when the accessory pathway is favored over the atrioventricular node, which can occur with atrial fibrillation or with the use of medications that block atrioventricular nodal conduction. Both scenarios are potentially life-threatening since they can precipitate ventricular fibrillation. In this patient, an electrophysiological study showed a right paraseptal accessory pathway anterior to the coronary-sinus ostium, which was successfully ablated. In the following 18 months, the patient had no further palpitations or identified episodes of preexcited atrial fibrillation.

