

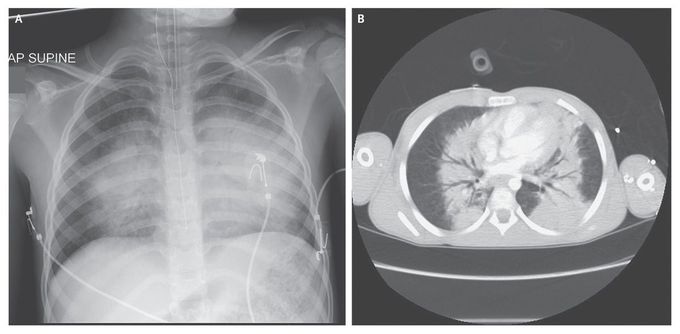
Blast Lung
An 8-year-old boy was injured when an improvised explosive device (IED) detonated very close to him. He had multiple wounds to his face, chest, abdomen, legs, and right arm caused by fragments from the IED. He was intubated en route to the hospital owing to airway obstruction and cardiovascular instability. Chest radiography (Panel A) and computed tomography (Panel B) revealed typical appearances of blast lung (pulmonary barotrauma), with interstitial and alveolar filling defects and prominent air bronchograms in a “butterfly” pattern. Lung-protective ventilation was provided with the use of a volume-controlled, pressure-limited mode. The partial pressure of arterial oxygen was normalized with ventilatory support, with a fraction of inspired oxygen of 0.4 to 0.6. Exploratory laparotomy revealed hemoperitoneum and multiple perforations of the small bowel and colon. Two days after the injury, the patient suddenly became hypoxemic and ventilation became extremely difficult. It was discovered that the tube was blocked by a large blood clot caused by pulmonary hemorrhage due to the blast lung. The endotracheal tube was replaced. The patient was successfully extubated after 1 week. On day 19, he was discharged home for palliative care after intestinal failure that was due to multiple small-bowel anastomotic breakdowns attributed to polytrauma and preexisting malnutrition. No further information was available after discharge.

