

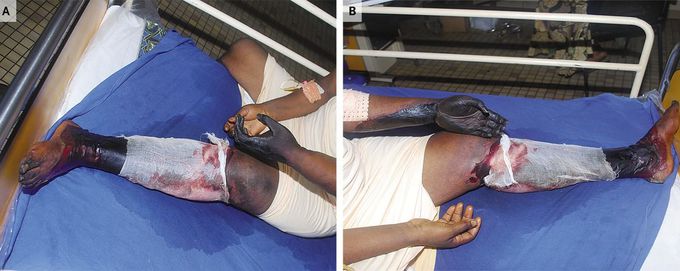
Simultaneous Gangrene of Both Left Extremities
A 47-year-old woman with a long history of diabetes mellitus, hypertension, and moderate obesity — with a body-mass index (the weight in kilograms divided by the square of the height in meters) of 34 — presented with a 1-week history of pain, paresthesia, pallor of the left arm and leg, and dry gangrene (Panels A and B). Neither a history nor a physical examination revealed evidence of a vasculitic, hypercoagulable, or embolic disorder. An ultrasound evaluation showed a thrombus of the distal two thirds of the left brachial artery and its bifurcation as well as a thrombus of the left external iliac and common femoral arteries. No definite source of the emboli was found, but an embolus from the heart released during a transient arrhythmia was suspected (she had no known history of atrial fibrillation, and her echocardiogram was normal). Balloon brachial and femoral thrombectomies and primary amputations were performed. During surgery, clots were found. The patient died a few days after surgery from the sepsis associated with the gangrene.

