

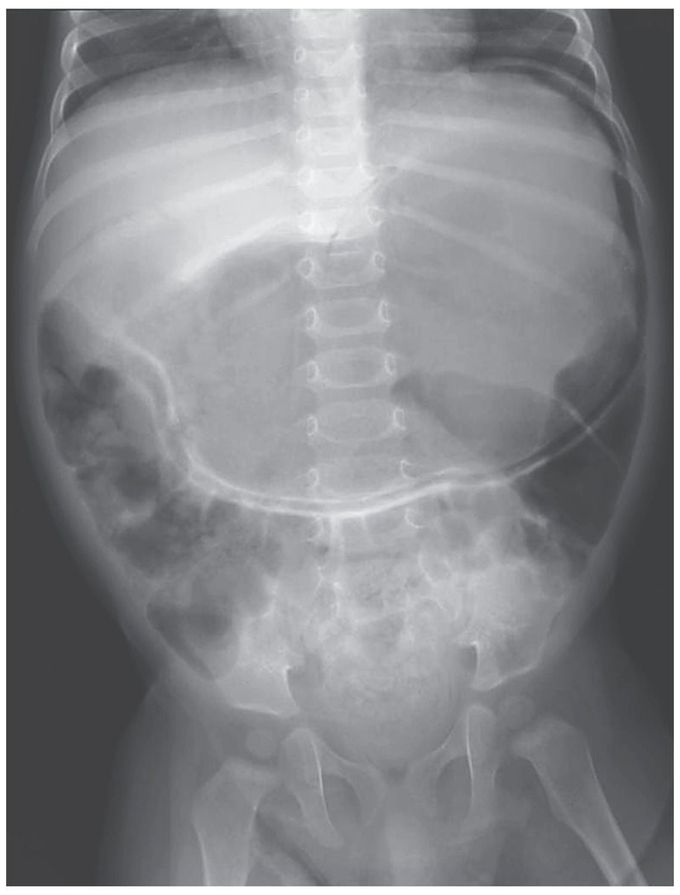
Gastric Emphysema
A 10-month-old male infant weighing 7.34 kg (2nd percentile for age and sex) presented with a 4-day history of nonbilious, nonbloody emesis. He had a history of frequent nonbilious emesis and poor weight gain since birth. He had difficulty consuming solid foods and was given a diagnosis of reflux. There was no surgical history. The patient's vital signs were normal, his white-cell count was 12,000 per cubic millimeter, and his abdomen was minimally distended, without tenderness. An abdominal radiograph showed marked gastric emphysema and some gas in the small bowel and colon. Abdominal ultrasonography and computed tomography, performed without the administration of contrast material, confirmed gastric emphysema with no obvious cause. The differential diagnosis included infection, ischemia, and gastric-outlet obstruction due to volvulus, annular pancreas, intestinal malrotation, and duodenal hematoma or stenosis. Laparotomy revealed diffuse gastric and omental emphysema resulting from duodenal stenosis. A duodenoduodenostomy was performed. Within 4 days after surgery, the patient was able to ingest formula and was discharged on day 6. A month later, he was eating age-appropriate foods without emesis.


