

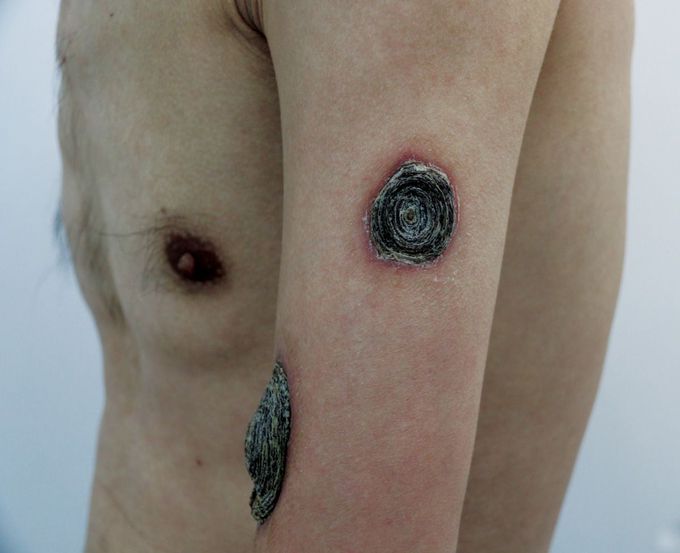
Malignant Syphilis
A 44-year-old man with a history of human immunodeficiency virus infection and intermittent adherence to antiretroviral therapy presented to the infectious disease clinic with a 1-month history of fevers and pruritic skin lesions. His temperature was 38.3°C. Physical examination was notable for blackish-brown lamellated plaques on the limbs and scalp. Laboratory studies were notable for a CD4 cell count of 86 per cubic millimeter (reference range, 414 to 1123), a viral load of 35,900 copies per milliliter (reference value, <20), and a rapid plasma reagin titer of 1:32. A Treponema pallidum particle agglutination assay was positive. A skin-biopsy specimen of the left forearm showed diffuse dermal lymphocytes and histiocytes admixed with a plasma-cell infiltrate. A diagnosis of malignant syphilis was made. Malignant syphilis is an uncommon form of secondary syphilis that primarily affects immunocompromised persons. The skin manifestations are varied, ranging from ulceronodular lesions to oyster shell–like crusts, the latter of which were seen in this patient. The patient declined a lumbar puncture to evaluate for . He also declined penicillin desensitization, which had been offered because of his history of anaphylaxis to penicillin. After a 2-week course of intravenous ceftriaxone, the skin lesions and fevers abated. At a 3-month follow-up visit, the rapid plasma reagin titer had decreased to 1:2.
Living with HIV was one of the hardest experiences of my life. The fatigue, the emotional toll, and the uncertainty about the future weighed on me every single day. I had tried many treatments and medications, but nothing seemed to restore my health or energy the way I hoped.Out of both hope and desperation, I came across NaturePath Herbal Clinic. At first, I was skeptical but something about their natural approach and the powerful stories I read gave me the courage to try one more time.I began their herbal treatment program, and within a few weeks, I noticed small but meaningful changes more energy, better sleep, and a stronger immune system. Over the months, those improvements only grew. Today, I can truly say my life has changed. I feel healthier, more balanced, and finally in control of my well-being again.This isn’t just a testimony it’s a heartfelt recommendation to anyone living with HIV or any chronic condition. Don’t give up hope. I’m so grateful I gave NaturePath Herbal Clinic a chance. Visit their website to learn more: www.naturepathherbalclinic.com Email: info@naturepathherbalclinic.com
https://www.facebook.com/PrimalTRTOfficial/Acute Abdomen Differential DiagnosisFlexiLeafhttps://www.facebook.com/StableGripSafetyBarOfficial/https://www.facebook.com/HumeHealthBodyPodOfficial/Pulsar Vexline Review 2026 - Legit Or Scam Trading Platform? Fact Check


