

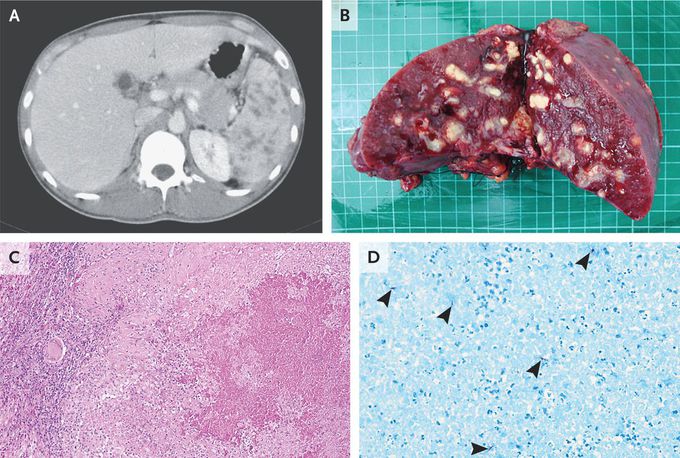
Splenic Tuberculosis
A 29-year-old man with human immunodeficiency virus (HIV) infection presented to the emergency department with a 2-week history of abdominal pain on the left side. Six months before presentation, he had received a diagnosis of HIV infection and non–drug-resistant pulmonary tuberculosis, for which antiretroviral and four-drug antituberculous therapy had been initiated. Soon after the diagnosis, however, his antituberculous regimen was reduced to rifampin and isoniazid only. At the current presentation, the left upper quadrant of the abdomen was tender to palpation. The CD4 cell count was 119 per cubic millimeter, and the viral load was 1778 copies per milliliter (reference value, <20). Computed tomography of the abdomen showed an enlarged spleen with numerous hypodense lesions (Panel A). A splenectomy was performed to evaluate for cancer. Gross examination of the spleen showed numerous necrotic nodules with purulent discharge (Panel B). A histopathological examination showed granulomatous inflammation with caseous necrosis (Panel C) and acid-fast bacilli (Panel D, arrowheads). A tissue culture was negative. Real-time polymerase-chain-reaction testing of the tissue identified Mycobacterium tuberculosis, which confirmed a diagnosis of splenic tuberculosis. Pyrazinamide and ethambutol were added back to the patient’s antituberculous regimen, and the patient completed 9 months of four-drug therapy.
Living with HIV was one of the hardest experiences of my life. The fatigue, the emotional toll, and the uncertainty about the future weighed on me every single day. I had tried many treatments and medications, but nothing seemed to restore my health or energy the way I hoped.Out of both hope and desperation, I came across NaturePath Herbal Clinic. At first, I was skeptical but something about their natural approach and the powerful stories I read gave me the courage to try one more time.I began their herbal treatment program, and within a few weeks, I noticed small but meaningful changes more energy, better sleep, and a stronger immune system. Over the months, those improvements only grew. Today, I can truly say my life has changed. I feel healthier, more balanced, and finally in control of my well-being again.This isn’t just a testimony it’s a heartfelt recommendation to anyone living with HIV or any chronic condition. Don’t give up hope. I’m so grateful I gave NaturePath Herbal Clinic a chance. Visit their website to learn more: www.naturepathherbalclinic.com Email: info@naturepathherbalclinic.com


