

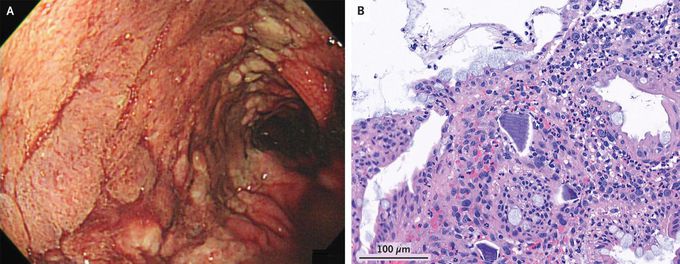
Calcium Polystyrene Sulfonate–Related Colonic Necrosis
A 58-year-old woman who was hospitalized for acute-on-chronic kidney injury had sudden-onset bloody stools. At the time of admission, she had had hyperkalemia, and calcium polystyrene sulfonate — a cation-exchange resin that binds potassium in the colon — had been administered multiple times per day throughout the first 6 days of hospitalization. On hospital day 6, large-volume, painless hematochezia developed, along with a substantial decrease in the hemoglobin level. A colonoscopy revealed a continuous ulcer extending from the splenic flexure to the rectum (Panel A). There was no active bleeding. A biopsy of the colonic mucosa showed epithelial injury and basophilic calcium polystyrene sulfonate crystals in a necroinflammatory background (Panel B). A diagnosis of calcium polystyrene sulfonate–related colonic necrosis was made. In rare cases, gastrointestinal injury may occur with the use of calcium polystyrene sulfonate or its analogue, sodium polystyrene sulfonate. The true frequency and underlying mechanism are not known. The colon is the most frequently involved site. The patient’s hematochezia resolved with cessation of the culprit medication and bowel rest. She was discharged on hospital day 45 with improved renal function and a normal potassium level.

