

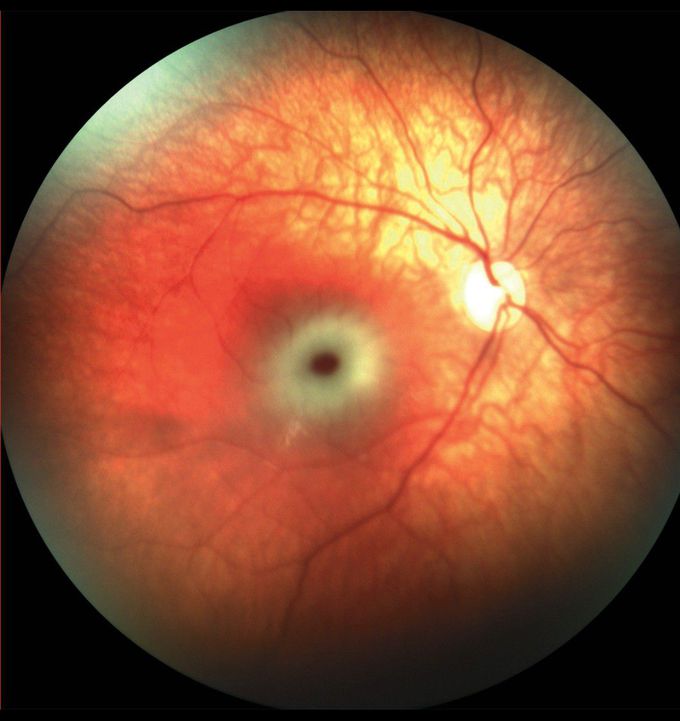
Cherry-Red Spot in Tay–Sachs Disease
An 8-month-old girl with strabismus and developmental delay was brought to the ophthalmology clinic. Physical examination was notable for macrocephaly, intermittent exotropia in the left eye, and hypotonia. A developmental history revealed all milestones to be at the 5-month-old level. Funduscopic examination showed macular cherry-red spots in both eyes. Referrals to the pediatric neurology and genetics departments were made. Magnetic resonance imaging of the brain revealed inadequate myelination diffusely and a thin corpus callosum. Whole-exome sequencing showed compound heterozygosity for pathogenic variants of the HEXA gene, a finding that confirmed a diagnosis of infantile Tay–Sachs disease. On prenatal genetic testing, the patient’s mother had been identified as a variant carrier, but her father had tested negative. After the patient’s diagnosis, however, the father was found to carry a novel variant. Tay–Sachs disease is an autosomal recessive lysosomal storage disorder that results in progressive neurodegeneration. The cherry-red spot is a characteristic finding, also found in other lysosomal storage disorders, that is caused by abnormally whitened, lipid-laden neurons surrounding and accentuating the color of the normal fovea. The patient was enrolled in a clinical trial of gene therapy but subsequently had seizures and developmental arrest.

