

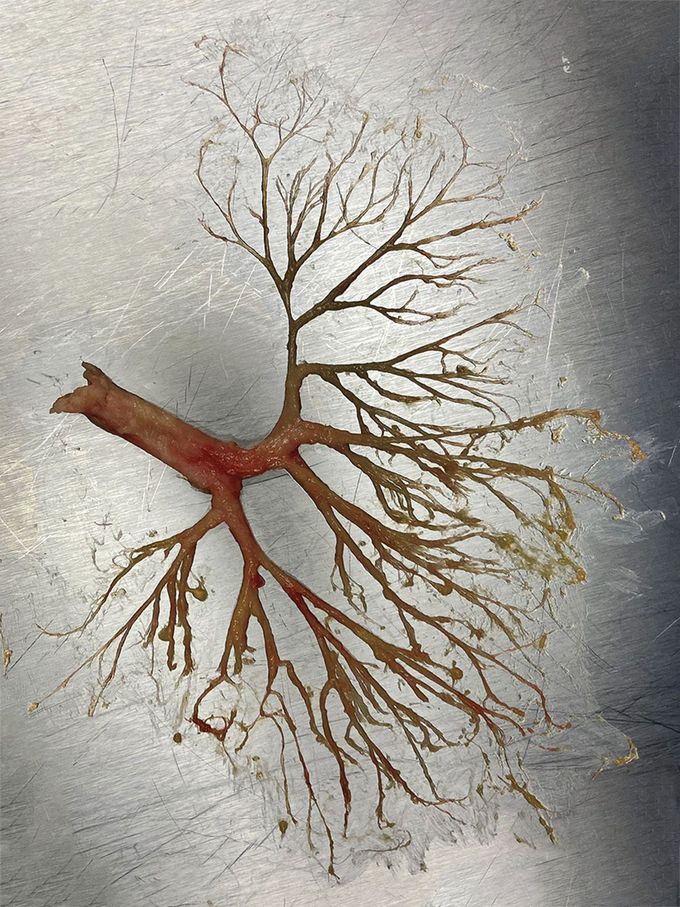
Plastic Bronchitis
A 50-year-old man with a history of alcohol-use disorder and rib fractures that had occurred 2 years earlier presented to the emergency department with stupor and hypercarbic respiratory failure. Intubation was performed. Breath sounds were diminished on lung auscultation, and a chest radiograph showed basal opacities in the lower lobes of both lungs that were later believed to be atelectasis on the basis of computed tomography (CT) of the chest. The next day, thick, white plugs were seen in the endotracheal tube, and complete collapse of the left lung was noted on a repeat chest radiograph on day 4. Bronchoscopy, performed on days 2, 3, and 4, initially showed multiple small, pale, rubbery, branching casts. The largest, observed in the left main-stem bronchus on day 4, extended to the subsegmental level and beyond. The patient’s spouse reported that he had been expectorating such casts for several months. CT showed only bibasilar atelectasis, and test results for infectious diseases were negative. Fibrin, mucus, and a mixed inflammatory infiltrate were observed on histopathological assessment of the casts. The patient received a diagnosis of plastic bronchitis, a rare condition that may be associated with surgical repair of the heart in patients with congenital heart disease, thoracic-duct trauma, sickle cell disease, and other systemic conditions. Serial cast removal was performed by means of bronchoscopy, and treatment with bronchodilators, mucolytic agents, and aerosolized tissue plasminogen activator was initiated. Extubation was performed 8 days after the start of treatment, and the patient was referred for further diagnostic testing, including magnetic resonance lymphangiography.

