

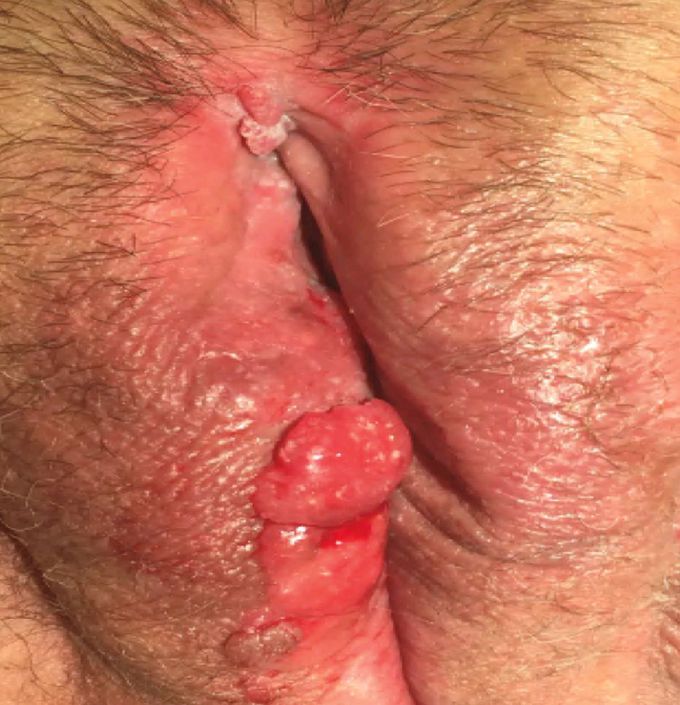
Vulvar Squamous-Cell Carcinoma
A 45-year-old woman was referred to the colposcopy clinic for evaluation of a wartlike lesion on her vulva. She reported having worsening pain and pruritus in the region during the preceding year. A vaginal swab obtained 2 months before presentation indicated candida vulvovaginitis, for which fungal treatment had been initiated, but her symptoms had not abated. She smoked cigarettes but had no history of abnormal Pap smears. On pelvic examination, there was a firm, tender lesion measuring 2 cm by 4 cm on the right labia majora and a smaller lesion at the anterior commissure of the vulva. The cervix and vagina were normal, and no palpable inguinal lymph nodes were noted. The anterior vulvar lesion was excised and found to be a high-grade squamous intraepithelial lesion. A punch-biopsy specimen of the labial lesion showed human papillomavirus associated with invasive vulvar squamous-cell carcinoma. She was referred to the gynecologic oncology department and underwent a radical right hemivulvectomy, with adjuvant radiation therapy for nodal involvement. At follow-up 2 years later, she remained cancer-free.

