

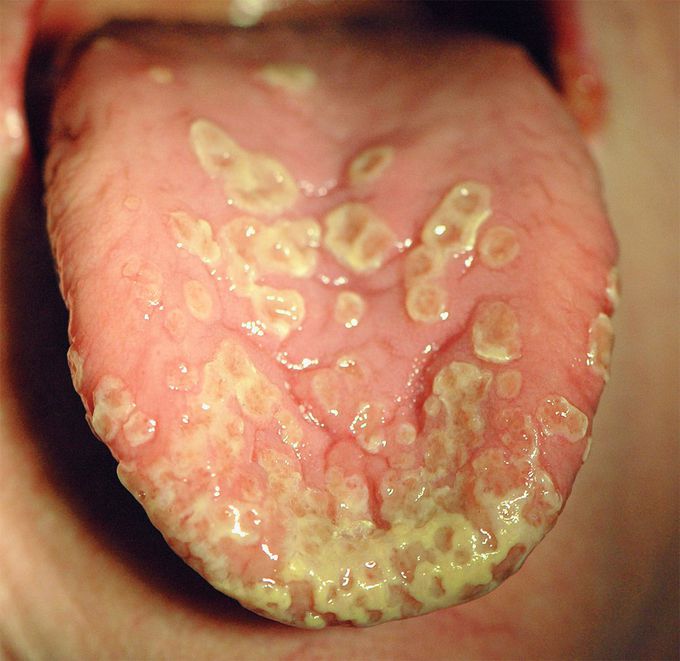
Pyostomatitis Vegetans
A 50-year-old woman presented to the dental clinic with a 10-day history of tongue and inner cheek pain. She had a history of Crohn’s disease, for which she had been previously treated with prednisone and mesalamine. At this presentation, she had no gastrointestinal or systemic symptoms. On physical examination, she had numerous painful, shallow erosions that merged to form linear “snail track” formations on the dorsal tongue and buccal mucosa. There were no skin lesions. Laboratory studies revealed an absolute eosinophil count of 870 per cubic millimeter (reference range, 50 to 500). A biopsy specimen of the dorsal tongue showed intraepithelial microabscesses with neutrophils and eosinophils, findings consistent with a diagnosis of pyostomatitis vegetans. Pyostomatitis vegetans is a rare oral mucosal condition that is most often associated with inflammatory bowel disease. The patient was referred for gastroenterologic evaluation, and her bowel disease was found to be quiescent. The oral lesions were treated with topical glucocorticoids and benzocaine. At 1 month of follow-up, her symptoms had resolved, and they did not subsequently recur.

