

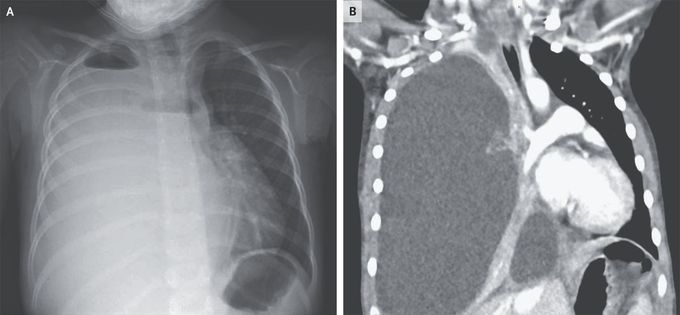
Pneumococcal Empyema
A 4-year-old girl was brought to the emergency department with a 4-day history of fever, cough, and lethargy. She was up to date with all childhood vaccinations. Three weeks earlier, she had had a presumed viral respiratory tract infection with fever and cough; testing for severe acute respiratory syndrome coronavirus 2 had been negative at that time. On arrival during the current presentation, she had a heart rate of 136 beats per minute, a respiratory rate of 32 breaths per minute, and an oxygen saturation of 92% while she was breathing ambient air. Auscultation of the lungs was notable for the absence of breath sounds on the right side and diminished breath sounds on the left. Laboratory studies showed a leukocyte count of 25,300 per cubic millimeter (reference range, 5000 to 15,500) with 88% neutrophils. Chest radiography revealed opacification of the right hemithorax with apical air–fluid levels, indicating the presence of a hydropneumothorax (Panel A). Findings on computed tomography of the chest included right lung collapse due to massive effusion and leftward mediastinal shift (Panel B). The left lung parenchyma appeared normal, without abscesses or cysts. The patient underwent chest-tube placement, and 1 liter of cloudy fluid was evacuated. Pleural fluid cultures grew Streptococcus pneumoniae. Pneumococcus remains an important cause of postviral pneumonia and empyema, even in fully vaccinated children. The patient received 14 days of treatment with ceftriaxone. At a 3-month follow-up visit, she had recovered fully, and a repeat chest radiograph was normal.

