An Icteric Tongue
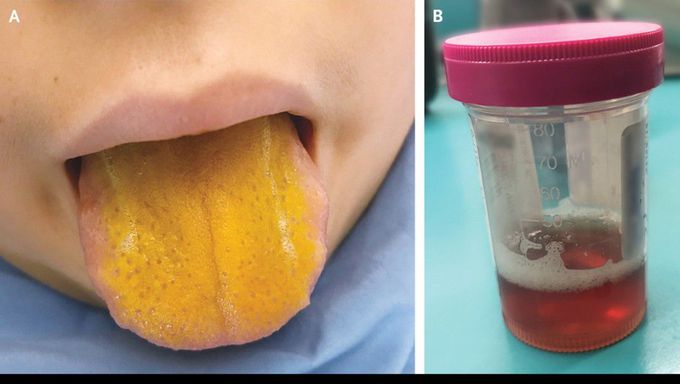
A 12-year-old boy was brought to the hospital with a 4-day history of sore throat and a 3-day history of dark urine, abdominal pain, and pallor. On examination he was found to have jaundice, with scleral and tongue icterus (Panel A) and dark urine (Panel B). Laboratory studies showed a hemoglobin level of 6.1 g per deciliter (reference range, 11.0 to 14.5), a lactate dehydrogenase level of 6405 U per liter (reference range, 470 to 750), and an unconjugated bilirubin level of 115 μmol per liter (6.7 mg per deciliter; reference value, <12 μmol per liter [<0.7 mg per deciliter]); a direct antiglobulin test was positive, with cold agglutinins detected. Urinalysis was positive for hemoglobin, and no granular casts or red cells were seen on microscopy. Testing for heterophile antibody was positive, as were qualitative polymerase-chain-reaction (PCR) and serologic tests for Epstein–Barr virus (EBV), with quantitative PCR showing a viral load of 36,000 IU per milliliter. A diagnosis of cold agglutinin, EBV-induced acute hemolytic anemia was made. The patient received a total of 5 units of packed red cells, as well as treatment with high-dose intravenous methylprednisolone for 2 days, followed by oral prednisone with a tapering dose over the next 7 weeks. After discharge, he recovered well, and the tongue icterus gradually resolved as the bilirubin levels normalized.