
Endoscopic endonasal surgery for giant pediatric craniopharyngioma
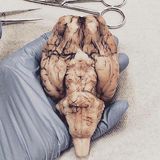
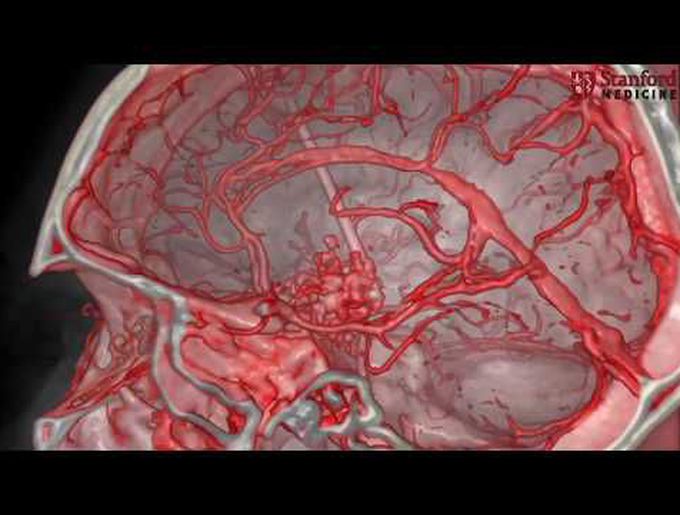
Pediatric craniopharyngiomas that were once thought to be inoperable or considered only for salvage medical therapy are now being reconsidered for aggressive surgical resection via endoscopic endonasal approaches. Here we review the operative video case of an 11-year-old with a giant complex craniopharyngioma that was resected via an endoscopic endonasal approach. Due to the extent of tumor burden near the basilar apex, a transclival approach was necessary. To accomplish this, a wide sphenoidotomy, posterior ethmoidectomy, and resection of the middle turbinate were necessary to create enough working space for the resection. We also highlight several key innovations in pediatric endoscopic endonasal surgery management and underscore a multidisciplinary approach that allows for the safe and successful treatment of these lesions. Our multidisciplinary team involves an experienced fellowship-trained endoscopic skull base surgeon and otolaryngologist, as well as a pediatric neurosurgeon, pediatric endocrinologist, pediatric anesthesiologist, and pediatric intensivists who play important roles in the preoperative, intraoperative, and postoperative phases of care of the patient. Finally, we discuss critical surgical decision points including pituitary transposition, which has a lot of conceptual appeal when it is anatomically feasible but unfortunately, in our experience, has low functional preservation rates. Initially, we always aim to utilize pituitary transposition for tuberoinfundibular craniopharyngiomas, and once the relationship between the tumor and the stalk is determined, a decision on whether to preserve or sacrifice the stalk and pituitary gland is made. In this particular case, there was a salvageable stalk and the transposition was performed knowing that the chances for functional preservation were low Ahmed Mohyeldin, MD, PhD,1 Peter Hwang, MD,2 Gerald A. Grant, MD,1,3 and Juan C. Fernandez-Miranda, MD1 Departments of 1Neurosurgery and 2Otolaryngology, Stanford University Medical Center, Palo Alto; and 3Pediatric Neurosurgery, Lucile Packard Children’s Hospital, Stanford, Palo Alto, California Include when citing: Published online April 1, 2020; DOI: http://thejns.org/doi/abs/10.3171/2020.4.FocusVid.19983 .

