

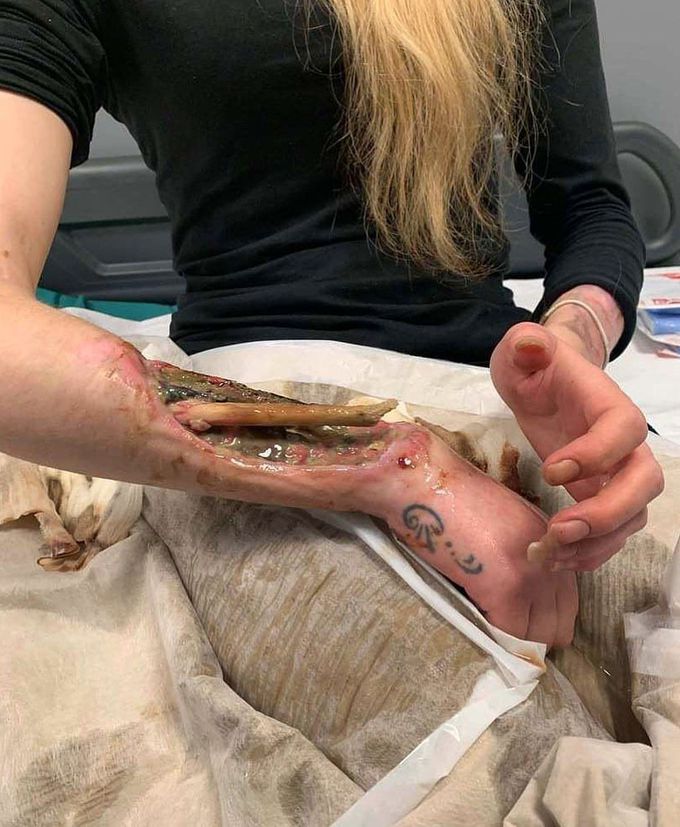
Severe skin necrosis with bone exposure in an IV drug user. Read about Krokodil drug below!
Skin and soft tissue bacterial infections are a common complication of intravenous drug use. This high rate is due to tissue death (necrosis) due to toxic materials in drugs and leakage of drugs out of veins during the injection (extravasation). Although skin infections usually present as areas of redness, warmth and tenderness (inflammation), the appearance in intravenous drug users is often atypical. This is because the skin, venous and lymphatic systems are damaged by the frequent penetration of the skin and consequent low-grade infection. Infections usually affect the arms or legs as these are the sites used most frequently for injection. Unusual sites may be involved (eg. abdomen, back, groin, scrotum and neck) due to injections in the jugular (neck) or femoral (groin) veins. One drug that can cause similar appearance is the Krokodil drug, a commonly used street name for desomorphine, an injectable opioid derivative that is associated with severe dermatologic effects. It’s a highly addictive substitute for heroin and it’s name is derived from crocodile (krokodil in Russian) and refers to the scaly, green-black skin discoloration frequently noted in its users. These patients present to the emergency department complaining of increased pain and swelling in the hands and forearms secondary to nonhealing ulcers. Usually, while they inject this substance, they notice a burning sensation during infusion. Patients later note gradual progression of the ulcers over several months, which eventually become malodorous with areas of necrosis. This ulceration can progress to severe muscle and cartilaginous tissue damage. Subsequent skin and muscle decay can cause the skin to slough off, often exposing the underling bone.

